This is a summary of the study setup and most important findings of a scientific paper focusing on health economics of Woulgan published in Journal of Wound Care (JWC) July 2019. It is part of our “In a nutshell” series where we report the basics of all the scientific papers making up the Evidence for Woulgan, to make the findings more accessible.
Type of study
The purpose of this study was to evaluate the cost-effectiveness of Woulgan as a short-term ad on therapy treating hard-to-heal wounds. The results were compared to patients treated with standard care from the previous year. The study was carried out in a UK community health care setting across four community general practitioner (GP) practices. You can read more of the clinical study the cost calculations were based on here.
Cost calculations
A treatment cost profile was constructed for each patient from information on the number and type of clinical contacts, dressings and other materials used for debridement and dressing changes, and prescriptions for analgesics and antibiotics. Any costs incurred before wounds became chronic/before enrolment were not included. Unit prices of dressings, prescriptions and other materials were derived from the NHS electronic drug tariff at January 2018 prices. The cost of Woulgan was £20 per tube, assuming single use per tube. The costs of clinical contacts were based on details of the resource use associated with wound care in the NHS in 2012/13 derived from an analysis of The Health Improvement Network (THIN) database. No patients in the current evaluation required specialist referral or a hospital outpatient visit, and clinical contacts were valued at a weighted average of practice nurse, community nurse and specialist nurse time.
Costs associated with the study was thus comprised of:
-
Cost for Nursing time at home or clinic derived from the THIN database
-
Cost for Materials used derived from NHS drug tariff
Table 1: Average cost per visit by contact type at 2013/14 prices, adapted from Guest et al. 2017
| Wound type | Practice nurse visits | Community nurse visit | Cost per nurse visit | GP visit | All contact types (excluding admissions) |
|---|---|---|---|---|---|
| Absess | £13.01 | £66.12 | £27.56 | £49.46 | £41.39 |
| Burn | £13.07 | £69.44 | £22.29 | £32.38 | £36.82 |
| Diabetic foot ulcers | £12.98 | £58.16 | £37.38 | £48.78 | £51.94 |
| Leg ulcer – arterial | £12.85 | £63.76 | £36.24 | £40.50 | £38.07 |
| Leg ulcer – mixed arterial and venous | £13.14 | £67.58 | £43.29 | £43.94 | £42.34 |
| Leg ulcer – venous | £13.00 | £62.51 | £28.45 | £49.25 | £36.35 |
| Pressure ulcer | £13.11 | £55.27 | £47.40 | £56.61 | £55.91 |
| Surgical wound | £12.98 | £63.87 | £28.69 | £44.10 | £41.21 |
| Trauma | £12.94 | £68.74 | £27.20 | £46.20 | £41.59 |
| Average case – weighted cost per clinical contact in current data |
£35.08 | £46.26 |
For full overview, click here.
Main findings
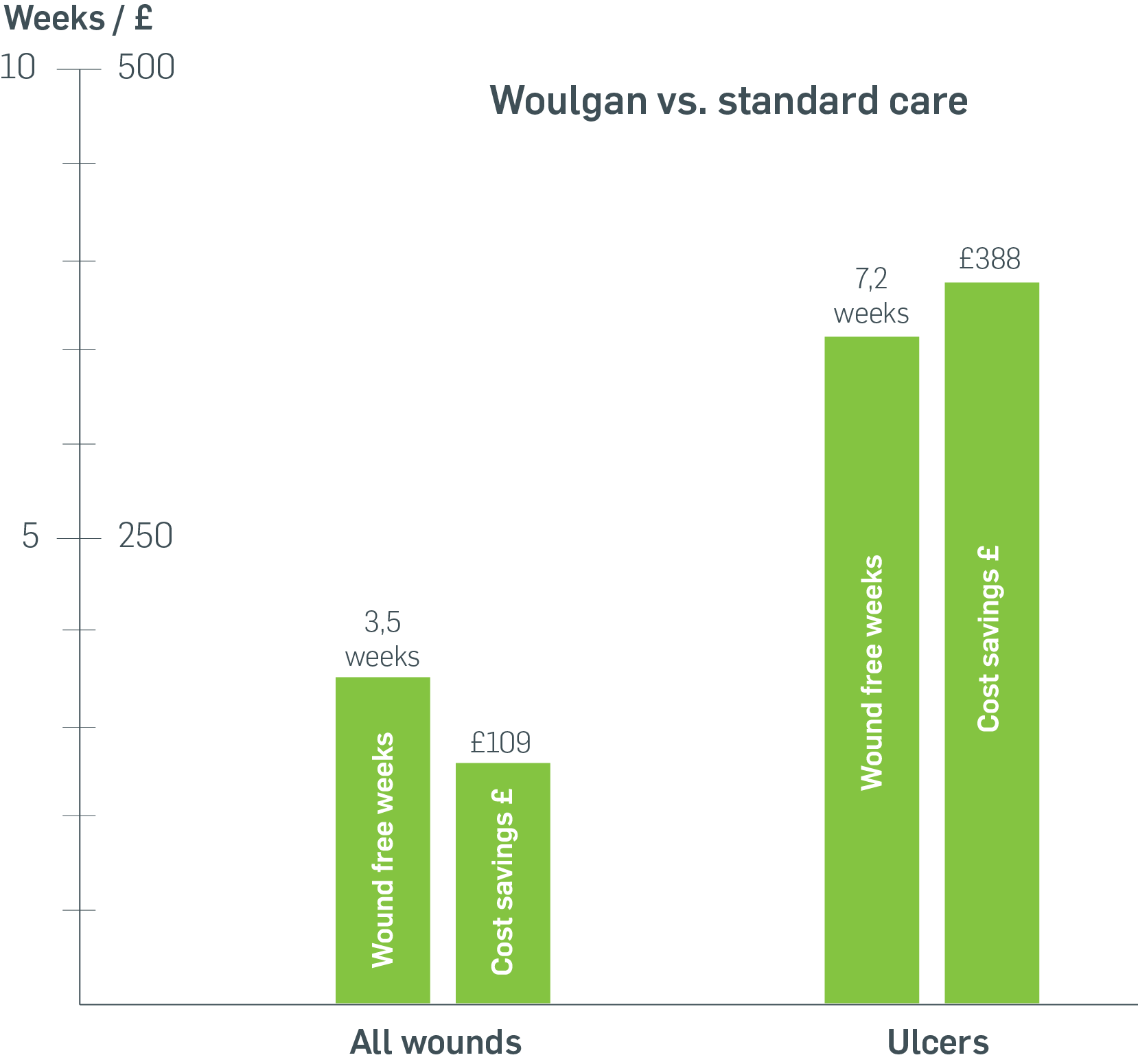
At week 12, the Woulgan group had a 91% healing rate compared to 66% in the standard care group. At 24 weeks, the Woulgan group had a 96% healing rate while the standard care group had 75%. The high rate of healed wounds in the Woulgan group resulted in more wound free weeks, thus fewer weeks of treatment for the patients. The results were even more pronounced when only including ulcer type wounds (DFUs, VLUs/ ALUs and PUs) from the study as opposed to the full cohort which also included acute wounds. The healing rates for ulcer type wounds were 92% for Woulgan vs. 46% for standard care at week 24. Improvement in healing was associated with a reduced mean number of weeks of treatment per patient and a reduction in the mean cost of treatment:
There were also more notable events in the standard care group that can spiral cost which were not costed in this study. This includes:
| Woulgan | Standard Care | |
|---|---|---|
| Amputations | 0 | 1 |
| Patients week with infection | 0 | 8 |
The study also included sensitivity analysis with both higher and lower costs for nursing time, these affected the total costs but still showed cost savings using Woulgan.
Tweet this: seven more ulcer free weeks after the use of @woulgan compared to standard care
Conclusions and limitations
The higher rate of wound healing in the Woulgan group implies that patients treated with Woulgan enjoyed more weeks with a healed wound and fewer weeks of treatment. Most of the lower cost was due to fewer clinical contacts. This evaluation was not an RCT, but a review of normal clinical standards using products available on prescription within the NHS. The lack of randomisation may be a limitation. On the other hand, the two groups were well matched at baseline and patients were treated according to the same standard care protocol and by the same clinical team. A caveat here is that the proportion of patients with offloading devices for a foot ulcer was significantly lower in the standard care group at 52% versus 83% (p=0.04), with four more patients receiving offloading in the Woulgan group versus the standard care group, and this may have affected the observed healing rates of this subgroup of ulcers. These results showed that short-term use of Woulgan on slow healing wounds can kick-start the healing process, shorten healing times, in addition to reduce NHS costs. As a result, patients can enjoy more wound free weeks, and quality of life will improve due to less time spent on wound treatment.
-
More wound free weeks for patient
-
Lower total costs for care
-
£388 per patient cost saving
-
Quality of life for patient improved