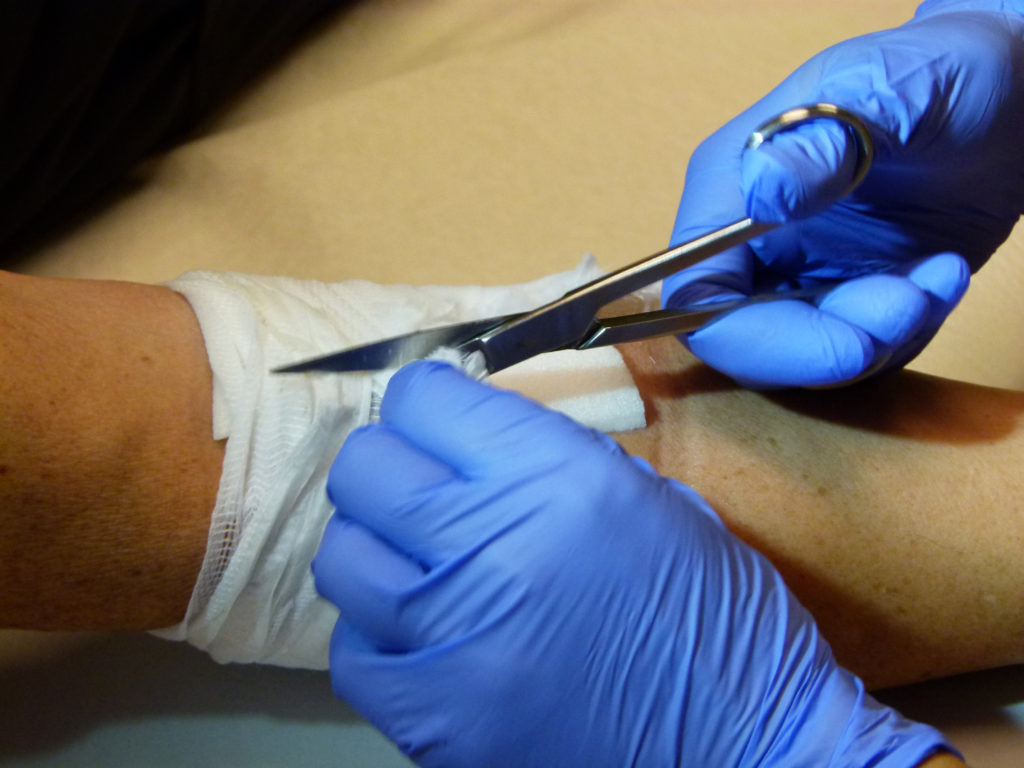
The Woulgan team has been lucky to get the chance to talk to nurse and midwife Christina Gamst at Tromsdalen medical practice, a general practitioner unit in Tromsø, Norway.
Organisation/History
Tromsdalen medical practice is a GP collective consisting of 6 physicians with about 9000 assigned patients. Their staff consists of 3 medical employees, which in Norway are the usual medical assisting staff at practitioner’s offices, and 2 nurses, whereof one is also a trained midwife. There are fewer GP units who employ their own nurses and/or midwives. The medical practice in Tromsdalen was opened in May 1998 and the first nurse was employed in 2012.
Tasks
Christina became a trained nurse in 2000 and midwife in 2010. She has a broad experience through assignments at the local emergency unit, a children’s ward, a health centre, a nursing home, a prison and a delivery ward. As a nurse at this GP collective, she is responsible for patients in need of wound treatment and minor surgery.

“Over the years I have done a few courses in wound care and think that it is a very interesting discipline which comes with constant changes and innovations so it is important to keep up”, Christina says. Apart from that, she assists the doctors with nursing tasks and the medical employees with dispensing medicine, since they are not authorized to do this themselves. She is also of assistance to patients with skin conditions like rashes and the like.
She tells us furthermore that she, as midwife, too is responsible for prenatal care of the pregnant patients at the medical practice. Her tasks have expanded in this sector over time. She thus offers help and guidance around contraception questions, and patients can also have her take a cervical smear test if they would rather have a midwife than a doctor doing the test.
Wound Consultations
“Acute wounds and traumata are usually quite simple to treat through cleaning well and stitching them if need be. Challenges appear when the wound does not heal. This applies to both acute and chronic wounds which stall during healing. In such a case, I have to develop wound care routines that align with the character of the wound, and possible other corrective actions. Usually when I develop a wound care routine, I re-evaluate it after about 4 weeks. If the wound healing did not make the progress I had hoped for, I have to think again and re-evaluate the treatment once more”, Christina tells us.
The wound patients she meets in her daily routine have post-operative wounds which do not heal as fast as they should; burns or diabetic wounds. In addition, she treats patients who have suffered a trauma which led to skin injuries. On average, she treats 2-4 wounds a week.
Collaboration
“Before I meet patients for the first time, they have been to a consultation at their doctor. Through collaboration we try to find the best solution. In cases where there is an infection, antibiotics need to be prescribed by the doctor. There can also be the need for a sick note which the doctor hands out. The actual wound care routine and choice of dressings is something I decide on”.
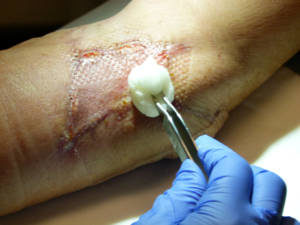
The practice receives several inquiries from home care providers. If it is possible with regard to the mobility of the patient, Christina takes the patient in and follows up on their treatment at the practice. In other cases, she develops wound care routines for the home care provider which they then follow up at the patient’s house.
“There are also patients who come from the hospital with routines we have to follow up on. In such a case, there is definitely a need for better communication than what we can find today. Some doctors at the hospital are however glad that we send them pictures of wounds to get guidance about further treatment, and to make sure we do not overlook something that should be followed up by them”, Christina says.
Ambitions
Christina is very involved with her wound patients and thinks that they should be met by qualified staff who knows all about the processes of wound healing and who can implement actions according to this knowledge. She says that she unfortunately often experiences somewhat of an incompetence which leads to poor wound care. There are for example a lot of dry dressings being used where they are absolutely inappropriate.
Other mistreatments include insufficient use of compression and an overuse of antibiotic treatments. “If the patient is met by health care professionals who are specialized in wound care, the chances for wound healing are much better. This saves the patient from unnecessarily lengthy treatments which could be avoided with the right choice of wound treatment option”.
The Ideal Situation

Based on her experiences, Christina would wish for more nurses to be employed at medical practices to safeguard the tasks she has described. She thinks that the transfer of knowledge is important and would want more wound courses to be held which would serve as a beneficial common platform for those interested in the discipline of wound care.
With so many people being involved with the patient, it is really important to improve the know-how of health care professionals. “Maybe we could get our own wound clinic in the municipality in the future?”, Christina concludes looking ahead.
Are you a wound nurse? Can you relate to Christina’s work routines and challenges? Tell us about your work life in a comment below!